Considerations Regarding the Use of Long-Acting Anxiolytics
Beers list warns that older adults have increased sensitivity to benzodiazepines and decreased metabolism of long-acting agents; in general, all benzodiazepines increase risk of cognitive impairment, delirium, falls, fractures, and motor vehicle crashes in older adults. If a benzodiazepine must be used, please consider utilizing a shorter-acting agent.
New Admissions and Anxiolytics
Many residents are admitted to a SNF/NF already on a psychotropic medication. The medication may have been started in the hospital or the community, which can make it challenging for the IDT to identify the indication for use. However, the attending physician in collaboration with the consultant pharmacist must re-evaluate the use of the psychotropic medication and consider whether or not the medication can be reduced or discontinued upon admission or soon after admission.
GDR Regulations
Within the first year in which a resident is admitted on a psychotropic medication or after the prescribing practitioner has initiated a psychotropic medication, the facility must attempt a GDR in two separate quarters (with at least one month between the attempts), unless clinically contraindicated. After the first year, a GDR must be attempted annually, unless clinically contraindicated. (CMS-F758)
References:
- “American Geriatrics Society 2019 Updated AGS Beers Criteria® for Potentially Inappropriate Medication Use in Older Adults.” Journal of the American Geriatrics Society, 29 Jan. 2019, pp. 1–21., doi:10.1111/jgs.15767.
- https://www.cms.gov/Regulations-and-Guidance/Guidance/Manuals/downloads/som107ap_pp_guidelines_ltcf.pdf
- Clinical Pharmacology. Accessed July 2020.
Treating Anxiety
Untreated anxiety can lead to cognitive impairment, disability, poor physical health, and poor quality of life. With anxiety disorders affecting as many as 20% of seniors, anxiolytics play a vital role in caring for your residents. There are both long-acting and short-intermediate acting anxiolytics. The charts below provide information on dosing, PO formulation, and FDA approved indications.
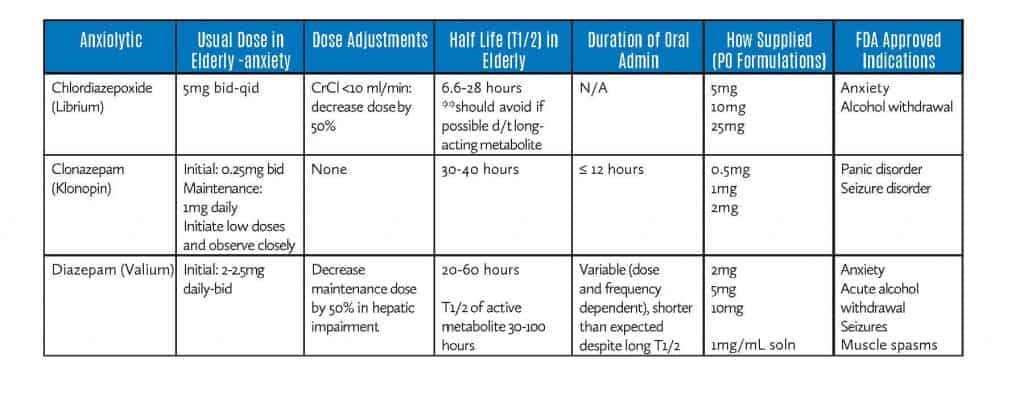
Long-Acting Anxiolytics
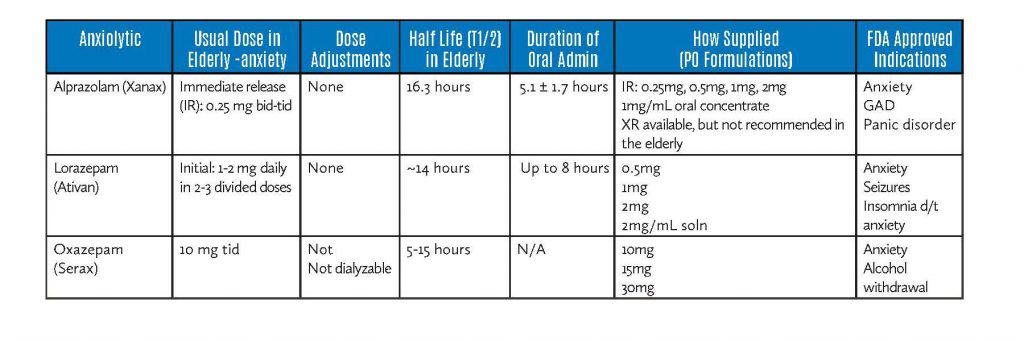
Short-Intermediate Acting Anxiolytics